Spring Issue Articles

By Michael J. Shea, PhD
In The Beginning
An infant’s first year is the most metabolically active time in the entire human lifespan. Extensive remodeling of the brain, lungs, heart and gut begin moments after birth. This happens intensively on many levels, from microcirculation and lipid conversion, to the proper filling of diapers. Microcirculation increases in the brain as the endothelium changes to accommodate the intensive growth of neurons. A vast network of capillaries expands throughout the body. High levels of cortisol and catecholamines are necessary for internal combustion of living on the land.
The lungs begin bringing oxygen into the blood and removing carbon dioxide from the blood at the level of the alvioli. The heart goes through extensive remodeling, not only in how endocardial cells function, but especially in the way that glucose is converted. Glucose is no longer stored in the heart as it was in utero, therefore the heart’s energy production must switch from glycolysis to lipid conversion. Intensive microcirculation occurs in the gut to accommodate oral nutrition.
The metabolic engine of life starts with the gut microbiome, acquired first from the mother’s body during pregnancy and birth and then through breastfeeding and skin-to-skin contact. It takes approximately three days after birth for a mother’s milk to come in. Human babies are born with extra fluid and fat, and the baby utilizes these stores in its first three days. The infant relies upon its stored water for hydration, its copious brown fat for energy and lipid conversion. Prior to the arrival of mature breastmilk, the mother’s body provides tiny amounts of colostrum, a thick, sweet, immunologically rich substance.
First colostrum and several days later, breastmilk, supply living cells and prebiotics such as human milk oligosaccharides to facilitate the development of the infant’s gut microbiome, the base for metabolism throughout the lifespan and normal cognitive development. Gentle and knowledgeable treatment from biodynamic practitioners can support the newborn and family during this crucial, metabolically active time.
“Gentle and knowledgeable treatment from biodynamic practitioners can support the newborn and family during this crucial, metabolically active time”
A Metabolic Protocol
In order to support such dramatic metabolic growth throughout the body and especially these four organ systems, I have developed a protocol to assess and support the metabolism of a newborn baby, particularly through the cardiovascular system. This is not so much a set clinical protocol, it is more like a smorgasbord with many delightful offerings. In my classes this is taught as a linear sequence. Linear progression and set protocols work well for class outlines and published articles. But as experienced pediatric therapists know, once the infant arrives in the arms of a concerned parent, adaptation is necessary, and embodied compassion is essential. To facilitate this, I usually treat the mother before or with the infant. In this protocol, simple changes in hand placement and/ or attention make this possible.
We will now go through the sequence, starting with the feet and moving upwards. This protocol is presented as I teach it in class knowing that you will adapt to each family system. It is helpful to know the metabolic logic behind each palpation skill. Also, let yourself wonder what is happening inside the baby’s body at a deep level. The deep level is the metabolic level: the entire endocrine system. The endocrine system includes the endothelium of the blood vessels and the gut microbiome.
The Extremities
The most basic principle in biodynamic cardiovascular work is to work from  periphery to center. When possible with an infant, begin contact with one or both anterior and posterior tibial arteries. This is especially valuable with infants who have had their umbilical cord cut prematurely, a common obstetrical procedure (versus the evidenced-based and physiologically sound practice of ‘delayed cord clamping’). With early cord clamping, there is an estimated 20- 60% decrease in blood transfer from cord and placenta to the infant’s cardiovascular system.
periphery to center. When possible with an infant, begin contact with one or both anterior and posterior tibial arteries. This is especially valuable with infants who have had their umbilical cord cut prematurely, a common obstetrical procedure (versus the evidenced-based and physiologically sound practice of ‘delayed cord clamping’). With early cord clamping, there is an estimated 20- 60% decrease in blood transfer from cord and placenta to the infant’s cardiovascular system.
This may lead to hypovolemic shock. Immediate cord clamping is also directly related to anemia in the first year of life, which is a huge stressor on the infant’s metabolism. Gentle contact with the tibial arteries and the brachial arteries supports the resolution of hypovolemic shock and relaxation of the vascular tree.
Since there is extensive circulatory and metabolic remodeling happening in the heart and lungs, the infant’s extremities experience a loss of blood volume. Peripheral acrocyanosis, or blueish- purple hands and feet, is a normal (albeit colorful) finding in the newborn. The central core metabolism of the infant is hard at work with a heart rate often twice that of an adult.
Normal infant heart rate:
Neonate (less than 28 days) Awake: 100-205 BPM, Sleep: 90-160 BPM Infant (1 month-1 year) Awake: 100-190 BPM, Sleep: 90-160 BPM Toddler (1-2 year) Awake: 98-140 BPM, Sleep: 80-120 BPM
Thermal Regulation
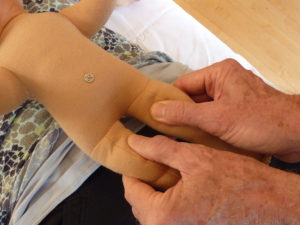 Another crucial metabolic function in a newborn is thermal regulation. Skin- to-skin contact (SSC) with a caregiver supports this function. When a baby is held by a caregiver, physiologically and metabolically there are two interconnected thermal systems, the
Another crucial metabolic function in a newborn is thermal regulation. Skin- to-skin contact (SSC) with a caregiver supports this function. When a baby is held by a caregiver, physiologically and metabolically there are two interconnected thermal systems, the
parent’s and the child’s. Within the baby’s body, there are also two interconnected thermal systems, one is in the core of the body and the other is in the extremities. These are connected via the cardiovascular system and the sympathetic nervous system (SNS) by regulation of blood flow, vessel wall dilation and contraction, especially in the capillaries.
Working biodynamically with the arteries of a newborn supports proper development of thermal regulation and the metabolism of the autonomic nervous system (ANS). Utilizing these contacts, the biodynamic practitioner, supports thermal regulation as the infant learns to integrate its two levels of thermal regulation, core and extremities.
Next, bilateral contact is made with the femoral arteries at midthigh in the 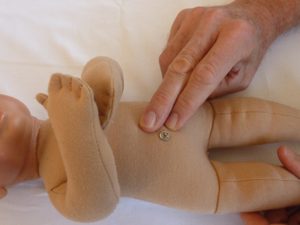 septum between the quadriceps and abductor muscles. In the adult I usually work ipsilaterally. This location is a Traditional Chinese Medicine (TCM) pulse location that supports proper blood flow to the pelvic floor for the function of urinating and defecating. Remember that full diapers in an infant are a really good thing. Gently using the thumbs, bilateral contact with the femoral arteries is quite easy to do on the infant’s body.
septum between the quadriceps and abductor muscles. In the adult I usually work ipsilaterally. This location is a Traditional Chinese Medicine (TCM) pulse location that supports proper blood flow to the pelvic floor for the function of urinating and defecating. Remember that full diapers in an infant are a really good thing. Gently using the thumbs, bilateral contact with the femoral arteries is quite easy to do on the infant’s body.
The Gut
Regarding health and disease, the gut is the center of the body: from microcirculation and neurohormone production to microbiome diversity, gut health is essential. In order to support microcirculation in the small and large intestines, I place one hand palm up over the infant’s umbilicus to feel the infant breathing. This hand placement continues until the slow breath of 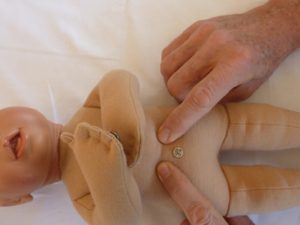 Primary Respiration is sensed through both my hand and the infant at the level of the umbilicus. Besides supporting microcirculation and respiratory integration, this also aids the wound healing of the umbilicus.
Primary Respiration is sensed through both my hand and the infant at the level of the umbilicus. Besides supporting microcirculation and respiratory integration, this also aids the wound healing of the umbilicus.
Next, I make gentle contact with one finger on the superior mesenteric artery (slightly above the umbilicus) and with another finger from the same hand, make contact with the inferior mesenteric artery ( just to the side of the umbilicus). The mesenteric arteries are linked to the SNS and are especially helpful for thermal regulation in the newborn. Thermal regulation in the abdomen is core thermal regulation. By supporting the microcirculation of the superior and inferior mesenteric arteries, two separate metabolic functions are being supported. One is core thermal regulation. The other is remodeling of the small and large intestine: substantial amounts of blood are being redirected into a vast endothelium forming in the center of this newly born body.
Then I make contact with the right and left colic arteries using the thumb and forefinger of one hand. The right colic artery is a main conduit of blood to the ascending and transverse colon. It derives from the superior mesenteric artery. The left colic artery is a main conduit of blood to the descending and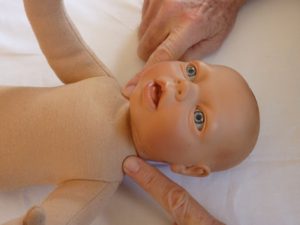 sigmoid colon, including the rectum. This simple contact is valuable in blending the function of these two arteries. In the distal portion of the transverse colon where the two mesenteric arteries overlap, is the overlap of the terminating point of the subdiaphragmatic vagus and the beginning of the sacral outflow of the parasympathetic nervous system. Therapeutically, this arterial contact offers a deep relaxing balance to the ANS. It supports the function of the subdiaphragmatic vagus that is monitoring blood glucose levels in the portal vein and liver.
sigmoid colon, including the rectum. This simple contact is valuable in blending the function of these two arteries. In the distal portion of the transverse colon where the two mesenteric arteries overlap, is the overlap of the terminating point of the subdiaphragmatic vagus and the beginning of the sacral outflow of the parasympathetic nervous system. Therapeutically, this arterial contact offers a deep relaxing balance to the ANS. It supports the function of the subdiaphragmatic vagus that is monitoring blood glucose levels in the portal vein and liver.
Along with microcirculation, the gut microbiome of the baby is being constructed. Beginning in utero, ignited at birth, then fueled with breastfeeding, snuggles and playtime, the process of human microbiome acquisition takes approximately two years. The parasympathetic function of vagal immobilization has an essential role in bladder and bowel function, especially in the newborn. The sub diaphragmatic vagus initiates communication between the gut microbiome with its immune and endocrine functions, the brain, and heart. The vagus monitors gut inflammation and sends these signals to the heart and brain.
This gut-central-vagal communication is foundational to an internal sense of safety while the brain of the newborn is oriented to an external sense of safety via the social nervous system that includes both the vagus nerve and the facial nerve. Such safety is an integral part of the formation of one’s body image, whether the infant loves their body, or struggles within it as if eternally flawed. The rapidly developing heart mediates these responses via its heart rate variability (HRV) and respiratory sinus arrhythmia (RSA). Thus, the heart juggles the internal and external safety in its basic function of vulnerability and openness to the environment. The heart can be easily imprinted in this intense metabolic remodeling. The house of the body is developed on a poor foundation.
The Neck
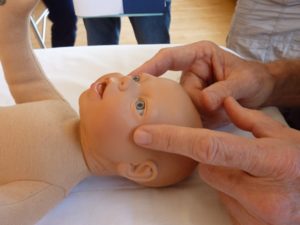
The next suggested contact is with the subclavian arteries. In our current culture, incredibly high levels of stress are endemic. Because of this it is important to approach the subclavian, a highly ANS innervated area of the body, gently and with great kindness. Since a baby’s body is small, it is possible to make bilateral contact with just thumb and index finger. However, in my experience, babies are very particular about contact around their heads and necks. At the beginning of a session, I introduce myself to the infant and figure out a communication style where I can negotiate permission to make contact and receive a “yes†or “noâ€. This could be anything from a nod of the head to a facial expression. At this point in the session, upon reaching the neck, re-establishing permission is important. With infants, as with most adults, I contact the subclavian arteries ipsilaterally and approach one side at a time. The ipsilateral approach offers a sense of safety to the wary contemporary client of any age.
Then I approach the carotid arteries. Once again contact is ipsilateral. Remember that the left carotid artery arises directly from the aorta, and the right carotid artery arises from the subclavian artery. Each artery has a very different sensibility and responsiveness to the slow breath of Primary Respiration. I like to differentiate the middle of the carotid artery. This is the carotid sinus where the carotid artery bifurcates into its external and internal branches. Located here is the carotid sinus baroreceptor, an important regulator of the ANS, innervated by the glossopharyngeal nerve. This baroreceptor is important in the regulation of blood pressure to the entire body including the carotid arteries provision of 80% of the total blood volume going to the brain and face. In the infant, the baroreceptors are doing crucial work: stabilizing peripheral and central blood pressures, regulating heart rate and variability, and coordinating cardiovascular functions with sleep and wake cycles.
The Cranium
On the rare occasion that I approach an infant at their head and face, it will be for contact with the temporal artery. This artery goes over the temporomandibular (TMJ) joint space and branches up into the temporalis muscle. This contact is supportive of the suck-swallow- breathe reflex. Optimal functioning of this reflex is crucial for an effective, efficient and enjoyable breastfeeding experience. The TMJ of a newborn is not a hinge joint. Suckling, whether at breast or bottle, requires that the mandible is able to glide forward, not just hinge down.
 The HeartÂ
The HeartÂ
Last in this teaching protocol but never least, is the heart. The most common contact I make with any baby is centering my palm around the fifth thoracic (T5) vertebrae on the child’s back. Never have I had a child refuse this contact; it seems to be both welcomed and deeply appreciated. I hold the child’s heart with the slow breath of Primary Respiration until I feel myself, my heart, the infant’s heart and their myocardium, all breathing with Primary Respiration.
If an infant is being held by his mother (or is playing on the floor or lying supine) I may place my hand palm up over the central portion of the sternum to feel the Fluid Body breathing. Often, while making this contact, I notice the feeling of a blessing being offered. Using my fingerpads, I connect with the valves of the heart, starting with the costosternal margin on the left third rib (R3) and finishing with the right costosternal margin of the fifth rib (R5). With fingers on the sternum in this diagonal line, the palm of the other hand can be placed at T5, supporting the back of the child’s heart. This contact is intended to synchronize the pulmonary valve, aortic valve, bicuspid (mitral) valve and tricuspid valve.
Conclusion
In conclusion, I will mention that if the mother/caregiver hands the baby to me, and if the baby is comfortable being held by me, I will receive the infant with one hand under its sacrum and my other hand supporting the baby’s occiput. With this dual hold, I sense the infant’s entire central nervous system breathing with Primary Respiration. This contact is especially lovely after treating the infant’s abdominal arteries. Through this dual hold, and the entire Neonatal Cardiometabolic Protocol as presented in this article, Biodynamic Craniosacral Therapy is applied to both the metabolic and physiological systems of the baby. With this work, we offer balance, stabilization, relaxation and normalization to the newborn human with the mother after their enormous work of gestating, birth, and transitioning to extrauterine life.
Acknowledgement
I owe a great debt of gratitude to K. Michelle Doyle. Michelle is a gifted midwife and biodynamic practitioner. She has been of enormous benefit to the world and her addition to the classroom where we teach together. She has greatly influenced this article.
Michael J Shea PhD obtained his master’s degree in Buddhist psychology at Naropa University in Boulder, Colorado, and a doctorate in somatic psychology at The Union Institute in Cincinnati, Ohio. He taught human embryology in the pre- and perinatal psychology doctoral programs at the Santa Barbara Graduate Institute in Santa Barbara, California, He is the author of several books: Biodynamic Craniosacral Therapy, Volumes 1-5 and Myofascial Release Therapy. He teaches Shamatha meditation classes around the world.  Michael is a member of the American Massage Therapy Association (AMTA) and has been a licensed massage therapist in Florida since 1976. He is a founding member of the International Affiliation of Biodynamic Trainings (IABT) and was a founding board member of the Biodynamic Craniosacral Therapy Association of North America (BCTA-NA). He lives in South Florida with his wife, Cathy, where they grow mangos, avocados and papayas. For more information visit his website: sheaheart.com.







